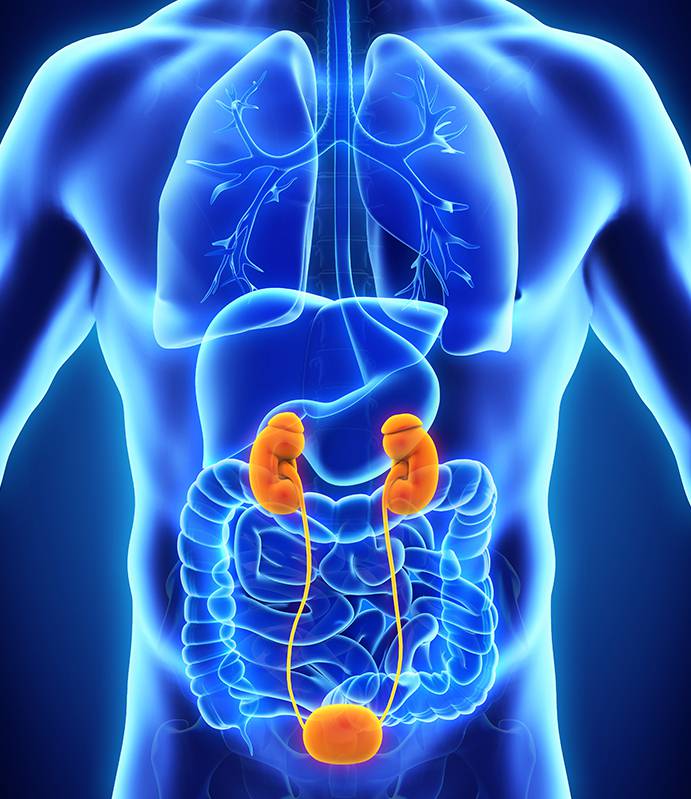
What is a vasectomy?
A vasectomy is a minor surgical procedure to cut and tie off the vasa deferens, which are the small tubes that carry sperm from the testes to the prostate. These can be accessed easily via small (3mm) incisions in the scrotum. This may be done under either local or general anaesthesia.
Who is suitable for a vasectomy?
This medical procedure is ideal for individuals who have made a conscious decision not to have children. It is also suitable for people who already have kids, but choose not to have more.
A vasectomy has to be considered an irreversible procedure. It is preferable that you are in a long term relationship and are sure that you have completed your family.
What are the benefits of vasectomy?
This form of permanent birth control offers many advantages, including:
- One-Time Cost – You only have to pay once when you go through a vasectomy. With other types of birth control, such as condoms and oral contraceptives, the expense accumulates with every purchase.
- Quick Procedure and Recovery Time – The procedure, in many cases, takes less than an hour to complete. Some patients may go home immediately after the surgery. Recovery periods will vary with each patient, but some may resume their normal activities one to two weeks following the vasectomy.
- No Long-Term and Adverse Effect on Sexual Pleasure – The medical procedure will neither diminish the intensity or duration of an orgasm nor affect the sensitivity of the penis.


What is the No Scalpel technique?
A urologist can perform this procedure in two ways: traditional vasectomy or no-scalpel vasectomy.
During a standard vasectomy, two incisions are made in the scrotum to allow the surgeon to reach each of the man’s vas deferens.
During a no-scalpel vasectomy, no incisions are made. Instead, the surgeon uses a hemostat (locking forceps with a sharp tip) to puncture through the skin of the scrotal sac. Then, the skin is gently spread only until both vas deferens can be visualized. Because the puncture site is so small and is just through the skin, stitches are usually not required and healing time is quick. As compared to a traditional vasectomy, the no-scalpel approach is a less invasive and quicker procedure.
How is the No Scalpel vasectomy done?
The goal during a no-scalpel vasectomy is the same as for a conventional vasectomy – to create a blockage in the vas deferens, so that sperm can no longer become part of the semen. This is done by cutting off a short piece of the vas deferens, removing it, and then ligating (tying-off), clipping or cauterizing (burning) the remaining vas ends.
An additional step of fascial interposition which consists of sewing connective tissue over the free prostatic end of vas (the end closest to the urethra) is also done. This creates a tissue barrier between the cut ends of the vas deferens. Some research suggests that this additional step decreases failure rates.
What about the “open ended” technique?
Men may be given the choice to have an “open-ended” procedure. This means that only the prostatic end of vas is tied or cauterized. The testicular end (closest to the testis) is left open. The reason for keeping this end open is to allow for sperm leakage.
Some research has shown that allowing for this leakage prevents the thickening or build-up of sperm because the sperm can flow into and be absorbed by the scrotum. This, in turn, can lead to less pressure -the potential cause of chronic post-vasectomy pain.
The open-ended technique has also been shown to lower complication rates as well as fewer cases of epididymitis (when the epididymis tube at the back of the testicle responsible for storing and carrying sperm becomes inflamed).