Varicocele
Feeling a dull ache in your scrotum or groin? Having difficulty fathering a child? These conditions may be caused by a varicocele!
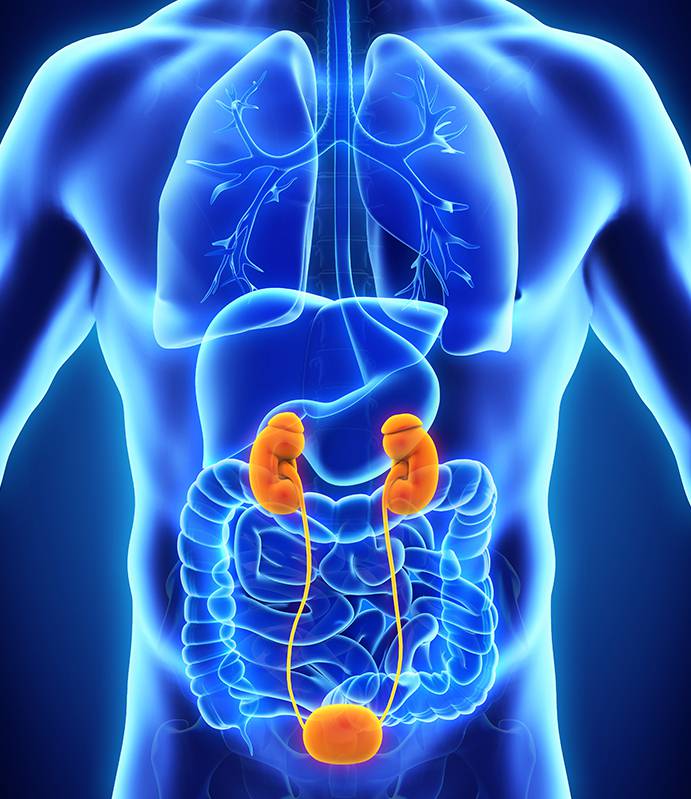
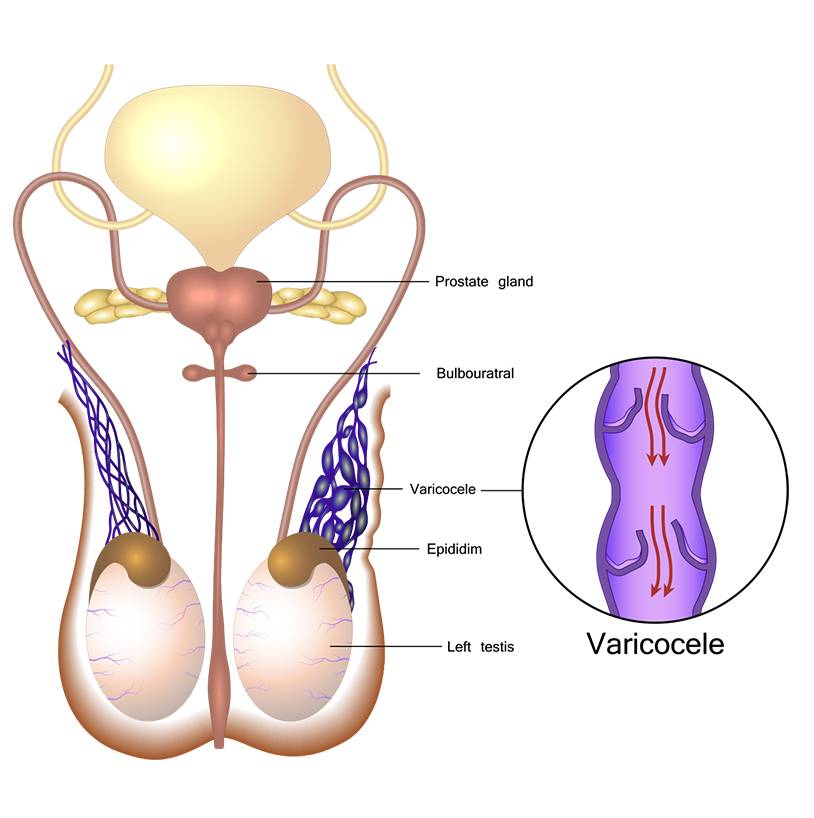
Figure 1 – Large varicoceles can look like a “bag of worms” externally. Valves in normal veins prevent backflow of blood. In varicoceles, defective valves allows backflow and pooling of blood, causing the veins to become wider and enlarged.
What is a varicocele?
Varicoceles are swollen and enlarged veins in the scrotum (Figure 1). These veins carry blood from
the testicles that are
low in oxygen and nutrients. Swelling can happen when defective valves in the veins allow blood to
flow backwards, and pooling of blood occurs in the veins. Varicoceles are similar to varicose
veins in the leg.
Most varicoceles are found only on the left side because of the
way blood drains from the left testicle. In some cases they can
also develop above the right or in both testicles.
Symptoms of Varicocele
A varicocele often produces no signs or symptoms. However, it might sometimes cause pain. The pain may:
- Vary from sharp to dull discomfort Increase with standing or physical exertion, especially over long periods
- Worsen over the course of a day
- Be relieved when you lie on your back
With time, varicoceles might enlarge and become more noticeable. A varicocele has been described as looking like a "bag of worms." The condition might cause a swollen testicle, more frequently on the left side. Repair of a varicocele may be considered when there is no other identifiable cause of the pain and the pain qualities are consistent with a varicocele, however there can be no guarantee that varicocele repair will eradicate the pain.
A varicocele may also cause:
- Shrinkage of the affected testicle (atrophy). Most of the testicle is made up of spermproducing tubules. When they are damaged, as from a varicocele, the testicle shrinks and softens.
- Problems fathering children (infertility). With a varicocele, the testicle may be too warm. This affects sperm formation, movement (motility), and function.
However, most men with a varicocele may have no fertility problems.
How is the Varicocele diagnosis made?
Your doctor will take a detailed medical history and ask questions about your symptoms, if any. Our doctor will carefully examine your genitals. A collection of swollen and tangled veins in the scrotum that can be felt more in the upright posture or during straining, suggests a varicocele. The swollen veins may feel like a “bag of worms”. Both testicles should be examined to compare their size. The testicle affected by varicocele may be smaller. Backward flow of blood (reflux) in the swollen testicular veins is usually confirmed by ultrasound of the scrotum.
Treatment of varicoceles
When Should a Varicocele Be Repaired? When there is:
- Pain, marked swelling, or physical discomfort likely caused by the varicocele is present
- OR The varicocele is impairing testicular/sperm function
Surgery
Microsurgical Varicocelectomy
A microsurgical varicocelectomy is performed under a high-powered operating microscope to achieve the
highest success rates with the lowest side effect risks.
This procedure is performed under general anaesthesia. An incision is made in the lower groin area, and
the spermatic cord is isolated. Each abnormal vein is meticulously dissected and tied off to disrupt
pooling of blood in the testicle and provide drainage of blood away from the testicle into healthy veins
draining into the pelvis.
Keys to a good operation are to interrupt every vein, leave every artery intact, leave the vas deferens
intact and leave lymphatic drainage intact. If an artery is cut, damage to the testicle can occur. If the
vas deferens is injured, sperm can be blocked. If lymphatics are cut, the scrotum can fill up with fluid
(hydrocele) and require additional surgery to drain the fluid.
The microsurgical approach has been statistically shown to reduce all of these risks compared to other
approaches.
For men with fertility issues, Microsurgical Varicocelectomy can significantly improve semen parameters
and allow for natural conception or lessen the need of reproductive assistance.
Varicocelectomy Surgery Time
The surgery lasts about 30-45 minutes per side so that a right and left procedure is typically performed as a day procedure or a single night stay in hospital.
Varicocele Surgery Recovery Period
Most men are able to return to normal, nonstrenuous activities after 2 days. As long as they are not uncomfortable, they may return to more strenuous activity, such as exercising, after 2–4 weeks. Pain from this surgery is usually mild but may continue for a few days. You will be prescribed pain medication for a limited time after surgery. Wearing briefs or a jockstrap can also help by relieving pressure in the testicles. It will take several months after surgery before improvements in sperm quality can be seen with a semen analysis. This is because it takes approximately 3 months for new sperm to develop.
Alternatives to Microsurgical Varicocelectomy
Varicocele Angiographic embolization
Small coils are introduced through a vein in the groin area
and are used to block the veins in the abdomen feeding the varicocele. This method does not
usually require you to be asleep (general anaesthesia) and is less invasive than laparoscopic
surgery. However, it uses X-ray, so you are exposed to radiation. The long-term success rates seem
to
be slightly lower compared to surgery, and treatment can
take more than one procedure.
However, there is no incision, so it is sometimes used in
patients with a previously failed surgical repair, pain as the main indication for surgery, and
body features that increase
the risk of surgery.
Laparoscopic varicocele ligation
A laparoscopic camera and small instruments are introduced to the abdomen, where the veins feeding
the varicocele are clipped.
This procedure has lower long-term success rates compared
to microsurgical varicocelectomy.
In addition, although complications are rare, when they do occur they can be far more serious than
other approaches.
Finally, the rate of hydrocele (collection of fluid around the testis) after surgery is higher
with this approach.