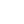MBBS, MRCS(EDIN), MMED(SURG), FRCS(UROL) (RCPSG), FAMS(UROL)

BSC(Monash), MBBS(NSW), FRCS(Glasgow), FRACS, MMED(Surgery), FAMS(Urol)

Urology surgery is commonly carried out to manage conditions affecting the urinary tract and male reproductive system, including kidney stones, prostate disorders and bladder conditions. Surgery is typically considered as an option when non-surgical treatments such as medication or lifestyle changes are no longer effective. A urology surgeon may then suggest surgery as a long-term solution to specific issues.
Understanding when surgery is needed and the types of procedures available can help you make informed decisions about your care. By becoming familiar with these common urology surgeries, you can better understand what to expect in circumstances where they are necessary.
When Might You Require Urology Surgery?
Urology surgery may be recommended when a condition progresses, causes significant discomfort or poses risks to overall health. While some urological issues can be managed conservatively, surgery often becomes necessary if you are affected by:
- Kidney stones that are too large to pass naturally or cause persistent pain or blockage
- Prostate conditions, including significant enlargement affecting urination or confirmed prostate cancer
- Bladder tumours or cancer, which require removal and further treatment
- Kidney tumours, where surgical removal is often needed to prevent spread
- Recurrent or severe urinary problems, such as ongoing obstruction or bleeding
In many cases, unusual symptoms are the first sign that something may be wrong. Persistent discomfort, changes in urination or abnormal findings should not be ignored. If you are experiencing these concerns, it may be time to see a urology surgeon for proper evaluation and guidance on whether surgical treatment is necessary.
Kidney and Urinary Tract Surgeries
Conditions affecting the kidneys and urinary tract can range from painful but benign issues like kidney stones to more serious concerns such as tumours or persistent urinary problems. Surgery is often focused on removing obstructions and treating disease.
Kidney Stones Treatment
Kidney stones are one of the most common urological conditions, often presenting with severe flank pain, blood in the urine or urinary obstruction. While smaller stones may pass on their own, larger stones or those causing persistent symptoms typically require surgical intervention.
Minimally invasive kidney stones treatment is aimed at physically breaking the stone into smaller pieces or removing it entirely. Depending on the size and location of the stone, this may involve inserting a small scope through the urinary tract to directly visualise the stone, followed by the use of lasers to fragment it into smaller pieces. In other cases, instruments may be used to retrieve the fragments or clear the blockage to restore urine flow.
Kidney Stones Shockwave Treatment (ESWL)
Extracorporeal Shockwave Lithotripsy, or ESWL, is a non-invasive variation of kidney stone treatment. Instead of inserting instruments into the body, high-energy shockwaves are directed from outside the body and focused onto the stone using imaging guidance.
These shockwaves travel through the skin and tissues without causing damage, but break the stone into smaller fragments upon impact. Over time, these fragments can naturally pass out during urination.
Kidney and Bladder Tumour Removal
Surgical procedures are occasionally needed to remove abnormal growths while preserving as much normal function as possible.
For kidney tumours, surgery is usually performed using minimally invasive or robotic-assisted techniques. Small incisions are made to insert surgical instruments and a camera, allowing the surgeon to precisely cut out the tumour from the kidney. In many cases, only the tumour and a small margin of surrounding tissue are removed, preserving the rest of the kidney.
For bladder tumours, removal is commonly performed through a transurethral approach. A thin scope is passed through the urethra into the bladder, allowing the surgeon to directly visualise the tumour. Special instruments are then used to shave or cut away the tumour from the bladder lining without any external incisions, reducing the recovery time and discomfort experienced.
Men’s Health Procedures
Certain urological procedures are performed to address men’s health needs, whether for contraception, medical conditions or personal reasons. These are typically straightforward procedures with well-established techniques and a relatively quick recovery time.
Vasectomy
A vasectomy is a minor surgical procedure performed for permanent male contraception. It involves blocking or sealing the vas deferens, the tubes that carry sperm from the testicles to the semen.
Using a no-scalpel technique, a small puncture is made in the scrotal skin to access the vas deferens. Each tube is then cut and sealed, usually with heat or clips, to prevent sperm from being included in the ejaculate. The procedure is typically done under local anaesthesia and does not affect hormone levels, sexual function or ejaculation, aside from the absence of sperm.
Recovery is generally quick, with mild discomfort or swelling for a few days.
Adult Circumcision
Adult circumcision is a procedure to remove the foreskin covering the head of the penis. It may be performed for medical reasons, such as a tight foreskin (phimosis), recurrent infections or hygiene concerns, as well as for personal preference.
The procedure is usually carried out under local or regional anaesthesia. The foreskin is carefully separated from the head of the penis and surgically removed, after which the remaining skin edges are sutured together. The area heals over a few weeks, during which patients are advised to keep the area clean and avoid strenuous activity.
Taking the Right Steps Towards Effective Urological Care
When symptoms of urological conditions persist, surgery can play an important role in long-term care. From minimally invasive techniques to men’s health surgeries, modern techniques are designed to improve treatment outcomes for patients while shortening recovery time and avoiding side effects.
If you are experiencing ongoing urinary issues, discomfort or have been advised about a potential condition, a medical consultation may help you understand your condition further and can help your doctor determine whether surgery might be an appropriate next step.
AtTan Urology, care is centred on clear diagnosis, thoughtful treatment planning and patient comfort at every stage. Dr Lincoln Tan, our consultant urologist, provides focused expertise in managing a wide range of urological conditions, with an emphasis on minimally invasive techniques and evidence-based care.
Contact us today to arrange a consultation and take the next step towards better urological health.
Meet Our Urologists

Dr Lincoln Tan
MBBS, MRCS(Edin), MMED(Surg), FRCS(Urol)(RCPSG), FAMS(Urol)
Dr Lincoln Tan is experienced in managing a wide range of urological conditions, with particular expertise in minimally invasive laparoscopic and robotic-assisted surgery. He is actively involved in advancing evidence-based approaches to improve diagnostic accuracy and clinical decision-making. As principal investigator in the first local study validating the Prostate Health Index for cancer risk assessment, he has contributed to reducing unnecessary biopsies and has been among the clinical leads introducing freehand, office-based transperineal biopsies in Singapore. Dr Tan is committed to comprehensive, patient-centred urological care.

Dr Robert Tan Tin Kiat
BSC(Monash), MBBS(NSW), FRCS(Glasgow), FRACS, MMED(Surgery), FAMS(Urol)
Dr Robert Tan has over 35 years of experience in the diagnosis and management of a wide range of urological conditions. As one of the first urologists in Singapore to perform transurethral resection of the prostate, he has played a key role in advancing minimally invasive urological care. A founding member of the Singapore Urological Association, Dr Tan is also a local pioneer in non-invasive urinary stone treatment, including extracorporeal shockwave lithotripsy. His practice emphasises careful assessment and personalised care supported by appropriate medical technology.